
Kris English, PhD
Professor Emeritus
University of Akron, Ohio US
In 1983, Donald Schön1 published a best-seller entitled The Reflective Practitioner: How Professionals Think in Action. His book explored “reflection-in-action” (or “in-the-moment”) problem-solving processes, as well as reflection-on-action (i.e., “after-the-moment”considerations). He framed reflection as an advanced learning process, involving the “exploration of experience, understanding its impact on oneself and others, and learning from this to inform future actions” (p. 481).2 His theories have been found to be applicable to virtually any profession, including healthcare and education.3-7
“Reflective practice” has since evolved to include not only an ongoing review of professional tasks, but also of personal interactions during those tasks. Audiologists can certainly relate to this dual experience: our appointments involve any number of patient-specific tasks while also engaging with the patient-as-person. “Task” details and “next steps” are clearly summarized in our clinical notes, readily available for review; however, although equally important, impressions of a patient’s engagement (trusting, skeptical, enthusiastic, resistant) may not be recorded, and could easily be minimized or forgotten. And yet it is fair to say that patient outcomes can heavily depend on the nature of our personal interactions.
Post-appointment or end-of-day reflections can help us review these relational dimensions. To that end, a validated 10-item self-report was recently designed to focus specifically on the provider-client encounter.8 The Reflective Practice Questionnaire (RPQ) “sets itself apart from other self-report reflection measures by predominately focusing on working with clients, and by utilizing broad phrasing so that the measure can be used across a wide range of professions where reflective practice is relevant” (p. 2). The RPQ is appropriate for professionals and students, and because it is brief, it meets the concerns of audiologists’ time constraints.

The authors have given blanket permission to reprint the RPQ.* (See statement at the end of this article.) A copy of the RPQ can be downloaded here: 10-Item RPQ.
Following are the questionnaire items, compressed into narrative form. Response options range from very rarely to almost always. Per audiology practices in the US, the term clients is replaced with patients.
Keeping the contexts of person-centered and equitable care at top of mind…
Items 1-4: During interactions with patients: I recognize when my pre-existing beliefs are influencing the interaction / I consider how my personal thoughts and feelings are influencing the interaction / I recognize when a patient’s pre-existing beliefs are influencing the interaction / I consider how their thoughts and feelings are influencing the interaction.
Items 5-8: After interacting with patients: I spend time thinking about what was said and done / I wonder about the patient’s experience of the interaction / I wonder about my own experience of the interaction / I think about how things went during the interaction.
Item 9: I think about how I might improve my ability to work with patients.
Item 10: I critically evaluate the strategies and techniques I use in my work with patients.
 Notably, these items prompt clinicians to reflect on how the encounter was experienced from the patient’s point of view as well as our own. Responses that include often, very often, and almost always are consistent with person-centered and equitable care. Responses ranging from very rarely, rarely, or sometimes suggest that we should explore personal barriers, biases, or inhibitions and, if appropriate, consult with a colleague or mentor for support. If our responses are not aligned with our person-centered, equitable goals, Campbell et al.9 recommend “…a variety of implicit bias mitigation strategies named in the literature. These include continuous reflection on one’s beliefs on specific social groups, gaining access to regular training, and seeking feedback from outside sources such as the (Implicit Association Test) IAT.” (p. 6).
Notably, these items prompt clinicians to reflect on how the encounter was experienced from the patient’s point of view as well as our own. Responses that include often, very often, and almost always are consistent with person-centered and equitable care. Responses ranging from very rarely, rarely, or sometimes suggest that we should explore personal barriers, biases, or inhibitions and, if appropriate, consult with a colleague or mentor for support. If our responses are not aligned with our person-centered, equitable goals, Campbell et al.9 recommend “…a variety of implicit bias mitigation strategies named in the literature. These include continuous reflection on one’s beliefs on specific social groups, gaining access to regular training, and seeking feedback from outside sources such as the (Implicit Association Test) IAT.” (p. 6).
Re: Continuous Reflection
A 2026 study demonstrates the need for continuous reflection. Gedeon et al.10 measured communication behaviors of 37 oncologists (24 White, 9 Asian, 4 of other ethnicities; none Black or African American) during encounters with two standardized patients: a White actor and a Black actor, both of same age and characteristics, and both trained to behave in identical manner during simulated clinical interactions. Using pre-established criteria, the researchers observed less time in patient engagement (by an average of 14 minutes), fewer questions, and less optimism, inclusion, and authenticity during “appointments” with the Black standardized patient. However, when surveyed later, the doctor-subjects were unaware of these disparities. Without continuous reflection (with subsequent insight and change), unequal care will continue to persist.
Conclusion
Given the many possible differences that can exist between audiologist and patient (ethnicity, race, sexual orientation, age, etc.), it may seem most efficient to focus solely on hearing issues. When we do so, however, we miss what patients want us to know and remember them as unique and valued persons. As Kazemi et al.11 predict:
The future of person-centered care lies not in further technical refinement but in reimagining care as a moral and relational process, i.e., as something created with rather than delivered to persons.
* From page 13: “The RPQ is free to use and there is no requirement to obtain permission from the authors for use. However, we do enjoy hearing from people about how they are using it and are always happy to receive emails letting us know what you are using it for, or any questions you may have.” (contact info: shane.rogers@ecu.edu.au)
References
- Schön D. (1983). The Reflective Practitioner: How Professionals Think in Action. New York, NY: Basic Books.
- Ooi SM et al. (2021). A systematic review of reflective practice questionnaires and scales for healthcare professionals: A narrative synthesis. Reflective Practice, 22(1), 1–15.
- Heydari S, Beigzadeh A. (2024). Medical students’ perspectives of reflection for their professional development. BMC Medical Education, 24(1), 1399.
- Mantzourani E et al. (2019). The role of reflective practice in healthcare professions: Next steps for pharmacy education and practice. Research in Social and Administrative Pharmacy, 15(12), 1476-1479.
- Taylor D. (2020). Reflective practice in the art and science of counselling: A scoping review. Psychotherapy and Counselling Journal of Australia 8(1).
- Machost H, Stains M. (2023). Reflective practices in education: A primer for practitioners. CBE—Life Sciences Education, 22(2), es2.
- Hernandez RA et al. (2013). Fostering students’ reflection about bias in healthcare: Cognitive dissonance and the role of personal and normative standards. Medical Teacher, 35(4), e1082-e1089. DOI: 10.3109/0142159X.2012.733453
- Rogers SL et al. (2024). Further development of the Reflective Practice Questionnaire. PeerJ, 12, e16879.
- Campbell CN. (2025). Healthcare inequities and healthcare providers: We are part of the problem. International Journal for Equity in Health, 24(1), 97.
- Gedeon C et al. (2026). Racial disparities in doctor-patient communication: Examining doctors’ encounters with black and white patients. Journal of Racial and Ethnic Health Disparities, 13:1783-1794.
- Kazemi A, Corlin TE. (2026). Person-centered care revisited: From problematizing its conceptual and methodological assumptions to proposing alternative foundations. International Journal of Nursing Studies, 176, 105325.

 Why Belonging Matters: A Human Need that Impacts QOL
Why Belonging Matters: A Human Need that Impacts QOL ways to communicate to patients that they unquestionably fully belong.17,18 Communicating belongingness “entails an unwavering commitment to not simply tolerating and respecting difference (which is no small thing in a world of violent othering), but to ensure that all people are welcome and feel that they belong in the society with agency and not as provisional guests”(p. 160).4
ways to communicate to patients that they unquestionably fully belong.17,18 Communicating belongingness “entails an unwavering commitment to not simply tolerating and respecting difference (which is no small thing in a world of violent othering), but to ensure that all people are welcome and feel that they belong in the society with agency and not as provisional guests”(p. 160).4 The Barometer measures “belonging” in five contexts (family, friend, workplace, local, national) – none directly applicable to experiences in a healthcare setting but a potential research project.
The Barometer measures “belonging” in five contexts (family, friend, workplace, local, national) – none directly applicable to experiences in a healthcare setting but a potential research project. For inspiration, consider
For inspiration, consider  Kirsten Ellis, BA, MSc, RHAD, AssocFBSA
Kirsten Ellis, BA, MSc, RHAD, AssocFBSA
 When audiologists share relatable stories or connect patients with support groups, they help individuals see that they are not alone in their journey. For audiologists, recognising common humanity means acknowledging that perfection is unattainable. Mistakes happen and challenges arise in clinical practice. By fostering a culture where vulnerability is accepted, audiologists can support each other and their patients more effectively.
When audiologists share relatable stories or connect patients with support groups, they help individuals see that they are not alone in their journey. For audiologists, recognising common humanity means acknowledging that perfection is unattainable. Mistakes happen and challenges arise in clinical practice. By fostering a culture where vulnerability is accepted, audiologists can support each other and their patients more effectively. Kris English, PhD
Kris English, PhD



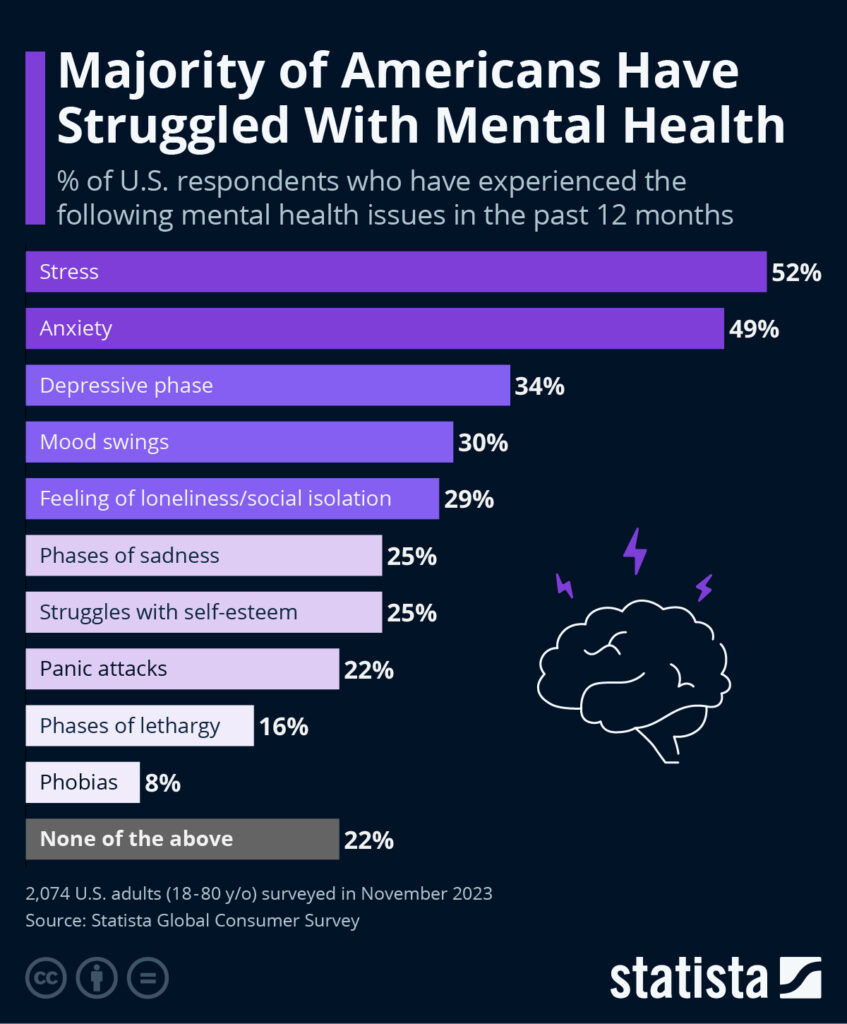
 Upskilling to an Essential Standard of Care
Upskilling to an Essential Standard of Care Taking the last question first: active listening is not about listening per se, but about interactivity. (It has been suggested that the term “conversational listening” might be more meaningful.1) While attending to a patient’s narrative, active listeners also verbally respond – with paraphrases, questions, affirmations, requests for clarifications, call-backs to previous topics – to assure patients that they are being heard.2,3
Taking the last question first: active listening is not about listening per se, but about interactivity. (It has been suggested that the term “conversational listening” might be more meaningful.1) While attending to a patient’s narrative, active listeners also verbally respond – with paraphrases, questions, affirmations, requests for clarifications, call-backs to previous topics – to assure patients that they are being heard.2,3


 Incongruence hinders our ability to communicate empathy and warm acceptance to persons associated with those biases, and efforts to do so come across as inauthentic.
Incongruence hinders our ability to communicate empathy and warm acceptance to persons associated with those biases, and efforts to do so come across as inauthentic. It would not be unusual for helping professionals to miss the impact of unconscious / implicit bias on congruence – even Carl Rogers seemed to have overlooked it until rather late in his career. Crisp8 recently reported on two video recordings of Rogers’ therapy sessions with two different Black male patients, conducted 5 years apart. The first session from 1979 was described by peers as having a “therapist-centric perspective” (p. 223) with missed opportunities to respond with empathy to the client’s racism experiences and avoiding an exploration about their racial and cultural differences.
It would not be unusual for helping professionals to miss the impact of unconscious / implicit bias on congruence – even Carl Rogers seemed to have overlooked it until rather late in his career. Crisp8 recently reported on two video recordings of Rogers’ therapy sessions with two different Black male patients, conducted 5 years apart. The first session from 1979 was described by peers as having a “therapist-centric perspective” (p. 223) with missed opportunities to respond with empathy to the client’s racism experiences and avoiding an exploration about their racial and cultural differences.






 Recently, an additional consideration of patients in the LGBTQ community receiving care in these settings indicated comparably positive PDQ results,12 but also raises a question: why wait until the end stage of healthcare? Social dignity violations (e.g., dismissal, disregard, grouping) routinely occur across a wide range of healthcare encounters throughout a lifetime.13-18 There seems no reason to wait: researchers very familiar with the PDQ have pointed out that the PDQ “can be used by any provider type and in numerous care settings to understand patient values” as a standard of care.19 Since all patients seek relational dignity throughout their lives, extending the PDQ intervention to all patients in all settings seems feasible, or at the minimum to those with historical concerns regarding inequitable care.
Recently, an additional consideration of patients in the LGBTQ community receiving care in these settings indicated comparably positive PDQ results,12 but also raises a question: why wait until the end stage of healthcare? Social dignity violations (e.g., dismissal, disregard, grouping) routinely occur across a wide range of healthcare encounters throughout a lifetime.13-18 There seems no reason to wait: researchers very familiar with the PDQ have pointed out that the PDQ “can be used by any provider type and in numerous care settings to understand patient values” as a standard of care.19 Since all patients seek relational dignity throughout their lives, extending the PDQ intervention to all patients in all settings seems feasible, or at the minimum to those with historical concerns regarding inequitable care.